You won’t find one “best” choice. Chiropractic can give quick relief for uncomplicated back flares via hands‑on adjustments. Physical therapy builds mobility, strength, and resilience to cut recurrences, using graded exercise and coaching. Research and guidelines favor staying active; manual therapy works best as an adjunct, not alone. Costs and time vary by insurance. Many people combine both—use adjustments to create a pain window, then load with targeted exercise. Next, you’ll see how to pick.
Key Takeaways
- Guidelines prioritize staying active and graded exercise; PT excels at progressive loading, motor control, and durable function gains.
- Chiropractic offers brief, hands-on adjustments that can provide quick, short‑term pain relief and flare control.
- Best outcomes often come from combining hands‑on care with an exercise program tailored to goals and tolerances.
- Evidence shows manipulation/mobilization provide small‑to‑moderate short‑term relief, comparable to other conservative care when dosing aligns.
- Choose based on goals, time, and risks; reassess progress within 2–4 weeks and address red flags immediately.
What Causes Back Pain and When to Seek Care
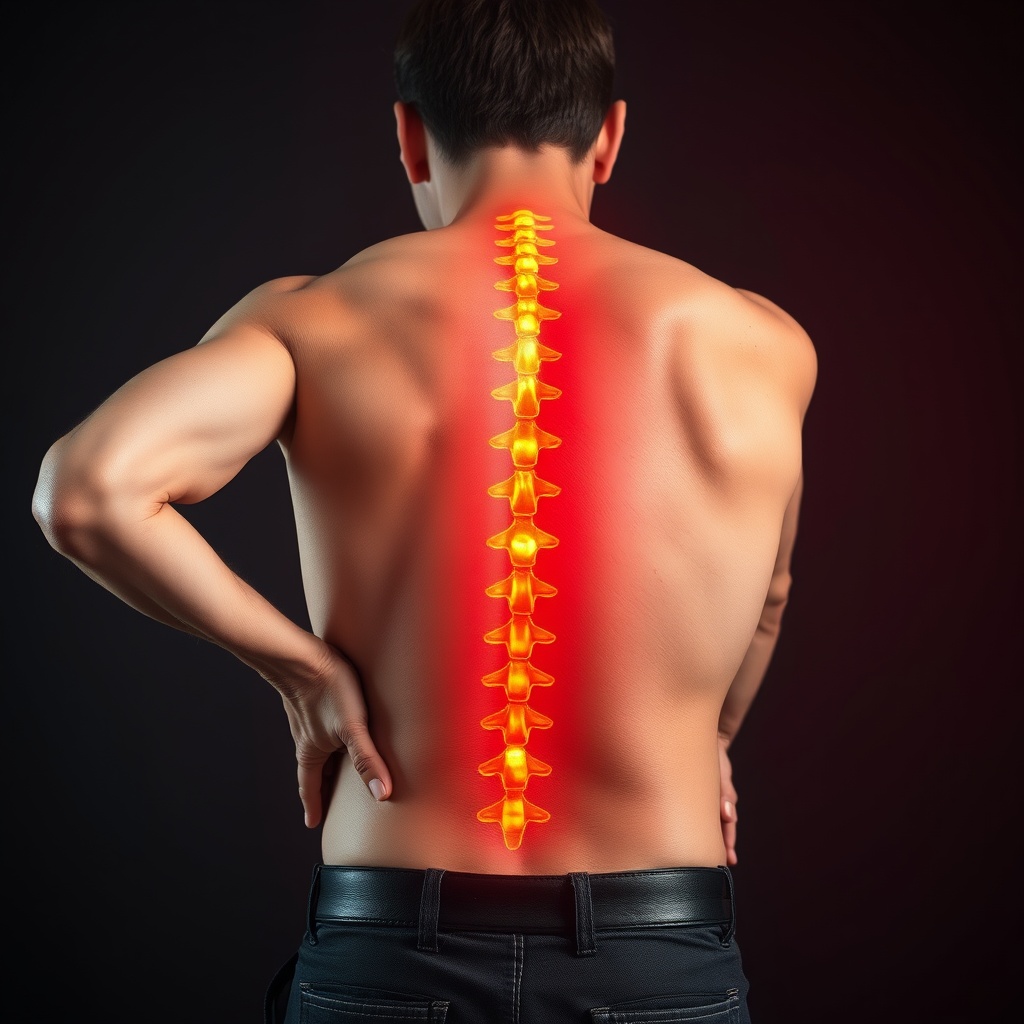
While back pain often stems from simple strains, it can also reflect issues in discs, joints, nerves, or underlying health conditions.
You might feel pain after heavy lifting, prolonged sitting, poor posture, or deconditioning.
Age-related changes like osteoarthritis or spinal stenosis can narrow spaces and irritate nerves.
Acute pain usually settles within weeks, but persistent or recurring pain often involves lifestyle, stress, and Psychosocial factors that amplify sensitivity.
Acute pain fades in weeks; ongoing pain often reflects lifestyle, stress, and psychosocial sensitivity.
Seek care urgently if you notice red flags: trauma, fever, unexplained weight loss, cancer history, steroid use, numbness in the groin, bladder or bowel changes, progressive weakness, or pain that wakes you at night.
Otherwise, consult a clinician when pain lasts more than 4–6 weeks, limits work or sleep, or keeps returning.
You can support recovery: keep moving as tolerated, use over-the-counter pain relief judiciously, practice Sleep hygiene, manage stress, and pace activities.
Early, informed action helps you prevent chronicity.
How Chiropractic Care Works
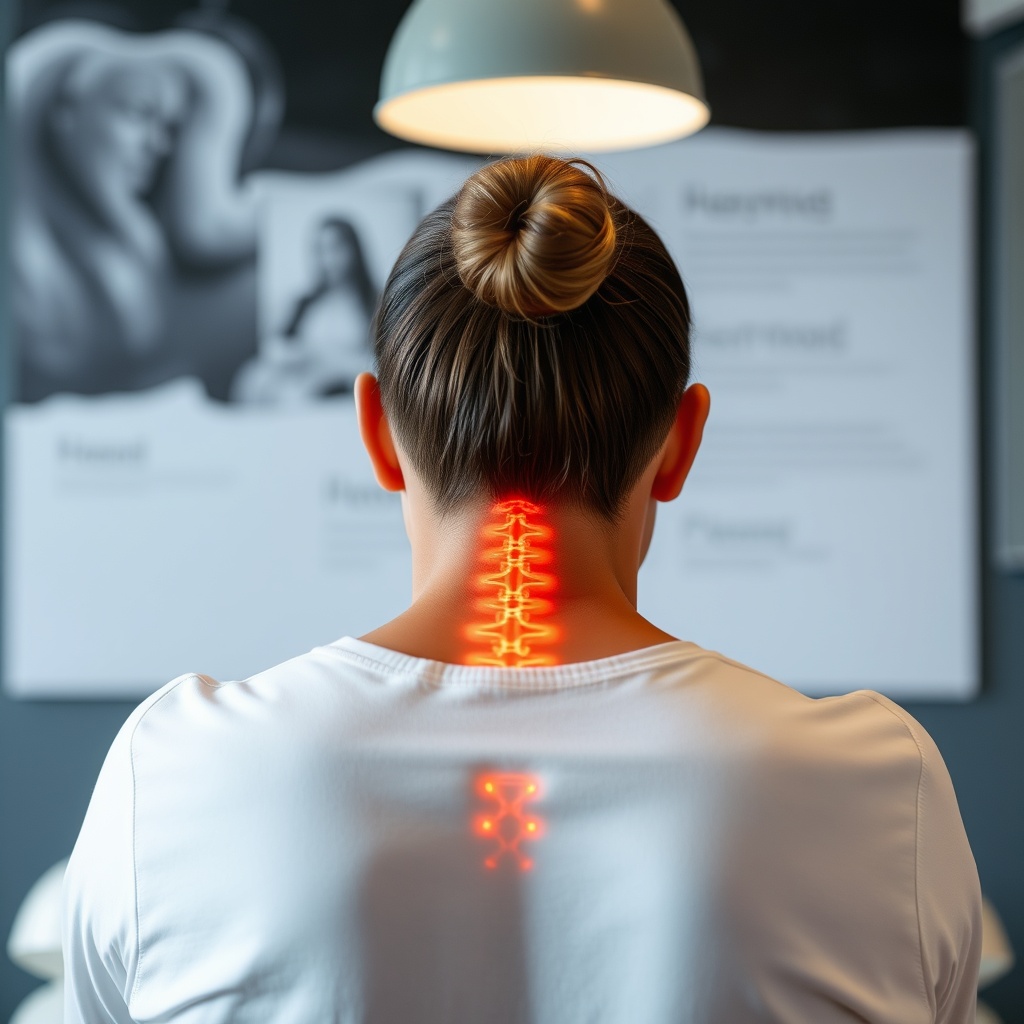
Because back pain often stems from restricted joint motion and irritated nerves, chiropractors first assess how your spine and nearby joints move, then target what’s stiff or sensitive.
They review your history, palpate joints and muscles, and may use simple orthopedic tests to pinpoint irritated tissues. Then they explain adjustment mechanics: a precise, low-amplitude, high-velocity thrust restores joint glide, briefly stretching capsules and influencing local receptors.
You might hear a pop as gas releases, but the goal is improved motion and reduced nociceptive signaling.
Care often includes gentle mobilization, soft‑tissue work, and home advice on posture and activity pacing.
Frequency depends on how you respond; many people notice easier movement within a few visits.
Chiropractic’s historical origins trace to late‑19th‑century manual medicine, but modern practice integrates anatomy, biomechanics, and safety screening.
Your chiropractor monitors progress, re-tests motion, and adjusts the plan so you gain relief while staying active.
How Physical Therapy Works
You’ll start with an assessment that sets clear, measurable goals for pain, mobility, and function.
Your therapist then builds a plan that progresses from basic activation to targeted strengthening and motor control.
As you hit milestones, they adjust exercise intensity, volume, and complexity to keep you advancing safely.
Assessment and Goals
Before treatment begins, a physical therapist performs a focused assessment to pinpoint what’s driving your pain and limiting your function. They listen to your history, observe posture and gait, test motion, and screen nerves. You’ll perform simple tasks to reveal irritants and tolerances. Together, you’ll use Goal Setting to define what matters—less pain, safer lifting, or restful sleep—and agree on timelines. Outcome Measures make progress visible, using tools like the Oswestry index, pain ratings, and timed sit‑to‑stand tests. The therapist then maps priorities, explains expected responses, and schedules reassessment to refine the plan.
| Focus | What it tells you | Example Outcome Measures |
| Pain behavior | Triggers, easing factors | NPRS, Oswestry |
| Function | Real‑life capacity | Sit‑to‑Stand, walking time |
You leave with clear priorities and a roadmap you understand.
Therapeutic Exercise Progression
Layering movement in the right order, a physical therapist builds your program from calm to challenge: restore mobility, groove motor control, then add strength, endurance, and finally speed or impact as needed.
You’ll start by easing stiffness with breath, gentle spinal mobility, and hip-opener drills.
Next, you’ll stabilize: practice neutral spine, diaphragmatic bracing, and hip hinge patterns.
Then you’ll load those patterns with progressive resistance, increase repetitions, and extend holds.
After that, you’ll build endurance with circuits and tempo work.
If your sport requires it, you’ll finish with power, impact control, and return-to-play tasks.
To stay on track, your therapist uses adherence strategies: clear goals, simple checklists, and habit anchors.
With technology integration—apps, wearables, and telehealth—you’ll get feedback, progression updates, and timely tweaks remotely.
Benefits and Limitations of Chiropractic Care
You may find chiropractic adjustments offer quick pain relief for some back, neck, and headache conditions.
But you should weigh potential risks—like soreness and rare nerve or vessel injury—and know it’s contraindicated with fractures, severe osteoporosis, spinal infections, or certain vascular disorders.
Understanding both sides helps you decide when chiropractic care fits your needs or when another approach is safer.
Pain Relief Potential
While spinal manipulation can quickly quiet some musculoskeletal pain, chiropractic care isn’t a cure‑all. You may feel noticeable relief in a few visits, especially for mechanical low back pain, but outcomes vary. Your Patient Expectations and the Placebo Effect can boost perceived improvement, yet lasting change usually depends on addressing movement habits, strength, and daily load. Chiropractors can reduce muscle guarding, improve joint motion, and coach you on pacing, but they can’t replace self‑management.
| Potential Benefit | Practical Limitation |
| Fast symptom easing | Relief may be short‑lived |
| Better movement awareness | Needs ongoing exercises |
| Hands‑on reassurance | Gains hinge on consistency |
Use care as a catalyst, not the sole solution; pair sessions with active strategies to extend pain relief. Track progress and adjust goals with your clinician regularly.
Risks and Contraindications
Because benefits come with trade-offs, chiropractic care carries risks that range from brief soreness, stiffness, fatigue, or headache to rare but serious complications after high‑velocity neck manipulation, including arterial injury and stroke.
You should avoid thrust adjustments if you’ve had recent fractures, spinal instability, cancer, infection, or new numbness, weakness, or bladder/bowel changes.
Severe osteoporosis, inflammatory arthritis, and vascular disease also raise risk.
Tell your chiropractor about blood thinners; anticoagulant interactions can increase bleeding or bruising from techniques.
Use pregnancy precautions: skip forceful manipulations, prone positioning, and excessive pelvic pressure; gentler, low‑force methods are safer.
If you have severe neck pain, dizziness, or headache after treatment, seek urgent care.
Prefer mobilization, exercise, and education when you want lower‑risk options, and coordinate with your clinician.
Benefits and Limitations of Physical Therapy
Although physical therapy builds strength, restores mobility, and reduces pain through targeted exercise, manual techniques, and education, it also demands time, consistency, and access to skilled providers. You’ll learn body mechanics, progress exercises, and get manual care when appropriate. Still, Practice variability means your experience can differ between clinics. Tele rehabilitation adoption helps when travel’s hard, but not every condition suits remote sessions. Insurance caps, schedules, and co-pays can slow momentum.
| Benefit | Limitation | What it means for you |
| Progressive loading builds resilience | Requires homework and regular visits | Commit to sessions and home exercise |
| Individualized plans target your drivers | Access varies by location and insurance | Ask about options and costs up front |
| Education prevents flare-ups | Remote care may miss hands-on cues | Use video well; request in-person checks |
If you want sustainable relief, PT equips you to manage flare-ups, not just mask pain. Expect gradual gains with consistent, guided effort.
Evidence and Guidelines: What Research Says
Across common musculoskeletal conditions, high-quality trials and major guidelines (ACP, NICE) converge on a few points: prioritize education to stay active and graded exercise; use manual therapy—spinal manipulation or mobilization—as an adjunct, not a stand‑alone; expect small-to-moderate, short‑term pain relief from manipulation comparable to other conservative care; and pair hands‑on care with exercise for better and more durable outcomes, especially for neck and low back pain.
For you, that means choose providers who coach self-management and prescribe progressive loading, not endless passive visits.
Evidence shows manipulation, mobilization, and exercise-based physical therapy yield similar benefits; track goals and function.
Note publication bias and guideline discrepancies: reviews favor one profession, but differences often reflect study design, dosing, or patient selection.
Prefer clinicians who measure outcomes, adjust plans within 2–4 weeks, and integrate activity, strength, and behavioral strategies.
Skip imaging; track sleep.
Combine approaches if it speeds return to normal life.
Risks, Safety, and Contraindications
Evidence favors active, active care; it also sets clear limits on safety.
You’ll get the most benefit when clinicians screen you for red flags—severe or progressive neurologic deficits, fever, trauma, cancer history, or osteoporosis.
Screening for red flags—deficits, fever, trauma, cancer, osteoporosis—maximizes benefit.
If any appear, you should avoid manipulation and seek urgent evaluation.
For routine low back pain, both chiropractic and physical therapy are safe, but risk differs by technique and your health status.
- Tell your provider about Medication interactions, blood thinners, and bone health; high-velocity thrusts may be contraindicated.
- Use Pregnancy precautions: avoid prone positioning, deep heat over the abdomen, and aggressive lumbar manipulations.
- New or worsening numbness, saddle anesthesia, or loss of bowel/bladder control demands immediate medical care, not conservative care.
- Recent surgery, spinal infection, fracture, or inflammatory arthritis often precludes manipulation; favor gentle, active exercise and education.
Ask about alternatives if you’re uneasy: mobilization, graded exercise, and motor control training carry low risk.
Cost, Insurance, and Time Commitment
While prices vary by region and insurance, you’ll usually pay less per visit for chiropractic care but spend more time per visit in physical therapy.
Chiropractors often charge lower cash fees and may bundle adjustments; PT clinics more often bill in timed units, which can add up.
Check your plan’s copay, deductible, visit caps, and referral rules.
Many insurers cover both, but network status and prior authorization can shift your out‑of‑pocket costs.
Ask for Billing Transparency: line‑item estimates, codes, and what’s applied to your deductible.
Time matters.
Chiropractic visits often run 10–20 minutes, 1–2 times weekly at first.
PT sessions typically last 40–60 minutes, with supervised exercise and home programs, 1–3 times weekly.
Factor Wait Times for first appointments; hospital‑based PTs can book out weeks, while some chiropractors offer same‑day slots.
Also consider travel time, parking, and missed work.
HSAs/FSAs usually cover both when medically necessary for care.
Choosing the Right Path: Who Benefits Most and When to Combine
If you’re dealing with acute, uncomplicated neck or low back pain, chiropractic care can deliver quick symptom relief via short, hands‑on adjustments.
When your goals include restoring strength, mobility, or sport performance, physical therapy’s exercise‑driven plan fits better.
If pain stems from joint stiffness and you’re healthy, start with a chiropractor.
If recurring episodes trace to hips, endurance, or post‑surgical needs, choose a physical therapist.
- Use chiropractic for brief, high‑frequency flare management; use PT to retrain movement, build capacity, and prevent relapse.
- Red flags (fever, trauma, numbness, bladder changes) warrant medical evaluation first, then guided rehab.
- Patient Preferences matter: comfort with manipulation, exercise intensity, and home program commitment shape outcomes.
- Combine when adjustments create a pain window that lets you load tissues safely with targeted exercises, with Care Coordination.
Reassess every two to four weeks. If progress stalls, switch emphasis or co‑manage with your providers and adjust goals.
Frequently Asked Questions
How Do I Verify My Provider’s Credentials and Licensure?
Check your provider’s license through your state board’s License Lookup, then confirm specialty credentials using Certification Verification on the certifying body’s site. Cross-check names, license numbers, expiration dates, disciplinary actions, and accreditation; don’t assume anything.
What Should I Wear or Bring to My First Appointment?
Wear Comfortable Clothing that lets you move easily and exposes your back if needed. Bring your Insurance Card, photo ID, medication list, imaging reports, referral, and questions. Arrive early. You’ll note symptoms, triggers, and goals.
Are Telehealth or Virtual Sessions Available for Back Pain Management?
Yes, clinics offer telehealth for back pain. You schedule video visits, use Virtual triage to prioritize symptoms, and ask follow-ups via Asynchronous messaging. Providers guide exercises, self-care, red-flag monitoring, and determine when in-person care’s necessary.
How Can I Maintain Progress While Traveling or Between Appointments?
You’ll maintain progress by sticking to simple Exercise routines, scheduling frequent Mobility breaks, and logging pain. Pack bands, walk daily, stretch after flights, mind posture, hydrate, sleep, and message your provider for tweaks between appointments.
Can They Provide Documentation for Workplace Accommodations or Activity Restrictions?
Yes, you can receive Medical Documentation outlining diagnoses, functional limits, and activity restrictions. Ask for details your employer needs, timelines, and updates. You’ll coordinate Return to Work plans, modify duties, and document progression safely together.
Conclusion
You’ve got options for back pain, and the best choice depends on your cause, goals, and timeline. Chiropractors can quickly ease joint-related pain; physical therapists build strength, mobility, and resilience. Evidence favors exercise-based rehab, with spinal manipulation helpful for short-term relief. Weigh risks, costs, and your schedule. If red flags appear, seek medical care first. Often, you’ll get the best results by combining approaches: use manipulation for relief, then commit to PT to prevent flare-ups.

